
Canada has legalized euthanasia and assisted suicide, known as medical assistance in dying (MAiD), under certain circumstances. These practices deliberately and intentionally cause a person’s death.
All human life is precious. Life is a gift from God for us to respect and protect through all its stages. As Christians, we believe that every person is made in God’s image (Gen 1:27) and loved by him (John 3:16). God is with us in our suffering and can redeem it (2 Cor 4: 7-12, 16-18). He is sovereign over life (Acts 17:24-26) and over death (1 Cor 15:20-28).
God calls us to care for those who are vulnerable, including those who are ill or near the end of life. The EFC supports palliative care as a compassionate response that supports and cares for those who are suffering or terminally ill.
Biblical principles such as respect for the dignity and sanctity of all human life, justice, and the care for those who are vulnerable are the basis of our opposition to euthanasia and assisted suicide.
Canada needs to prioritize treatment and support for Canadians - not facilitate or bring about their death.
Euthanasia & Assisted Suicide
This new brochure provides an update on MAiD in Canada, such as the upcoming change to allow MAiD for mental illness in 2027, the push for MAiD to be available to children and youth, and the need for there to be MAiD-free spaces.
Five key areas of concern on MAiD
1. MAiD on the basis of mental illness alone will take effect in March 2027. At a time when more Canadians are struggling with their mental health, mental health care isn’t available in a timely and affordable way for many Canadians and there is no clear way to distinguish between a desire for suicide and a request for MAiD. See a new opportunity to act by supporting
Bill C-218 and also our more general
brochure summarizing the issue.
2. Devastating impact on people with disabilities. MAiD can be an option for a person with a disability or chronic illness, even if the reason underlying their request is that they do not have adequate health care or social supports. People can also be pressured to end their lives via
MAiD because of their disability.
3. With MAiD’s subjective criteria, Canadians we would not expect to be eligible are having their lives ended by MAiD. Elastic terms, like “serious illness” and “reasonably foreseeable death”, could be
interpreted in subjective ways to mean a person who has up to a decade to live or someone who isn’t dying but does not want life preserving treatment. Health Canada’s annual report on MAiD deaths includes vision or hearing loss as conditions that have made someone eligible for MAiD.
4. There is a push for more expansion – to youth and by advance request. Advance requests set a very troubling precedent of ending the lives of people who are not able to consent at the time of death. A parliamentary committee has recommended allowing
MAiD for mature minors, youth under 18 years of age who are deemed capable of consenting. This would essentially remove the minimum age of eligibility.
5. The need for sanctuary. There is an urgent need for MAiD-free, safe places for patients and health care professionals where there is no pressure to end life via MAiD. There is pressure to
eliminate conscience protection for doctors and nurse practitioners for whom participation in MAiD is against their deeply held beliefs. We firmly believe doctors should not be the ones to suggest MAiD to patients.
New Resources
- Read and share the EFC’s updated brochures on the state of MAiD in Canada:
- See the EFC’s booklet on Palliative care: Palliative Care Toolkit
- Sign up for the EFC Update weekly newsletter, EFC daily social media feeds, and/or the EFC bimonthly newsletter Canada Watch
Other Resources
Why should we care about what’s happening and how does our faith shape our response to these issues? God calls us to care for our neighbour and to seek the well-being of our country.
We are stewards of this life, but it belongs to God. Christians believe God calls us to live the life He has given us. We do not need to accept medical treatment, but it is not for us to choose to intentionally bring about our death.
Fear and despair often fuel a request for assisted death. Many people are concerned about being a burden and may be afraid of what lies ahead. Government data shows that many people are choosing MAiD because of an inability to participate in meaningful activities, loss of dignity, feeling like a burden, and isolation or loneliness. The compassionate response is to support and encourage them, to provide high quality palliative care, not to end their lives.
God calls us to care for those who are vulnerable. To love our neighbour is the second greatest commandment, after loving God. Jesus’ parable of the Good Samaritan teaches that our neighbour is anyone who is in need.
"Open your mouth for the mute, for the rights of all who are destitute. Open your mouth, judge righteously, defend the rights of the poor and needy" (Proverbs 31: 8-9).
In both the Old and New Testaments, the people of Israel and followers of Jesus were commanded to care for the foreigner, the widow, the orphan and the poor. Another parable tells us that when we serve those who are vulnerable in our society, we are serving Christ (Matthew 25:34-36).
We must care for those:
- Living with a disability or serious physical or mental illness
- Struggling to receive proper medical care, economic or social supports
- In despair, believing their lives aren’t worth living
- Afraid of losing capacity or afraid they may suffer
- Needing pain control or support, but unable to access quality palliative care
We must affirm the value and dignity of every human life with compassion. The suffering experienced by many living with illness or disability does demand a response. We believe the compassionate response is to offer support and encouragement, to provide high quality palliative care, not to end their lives.
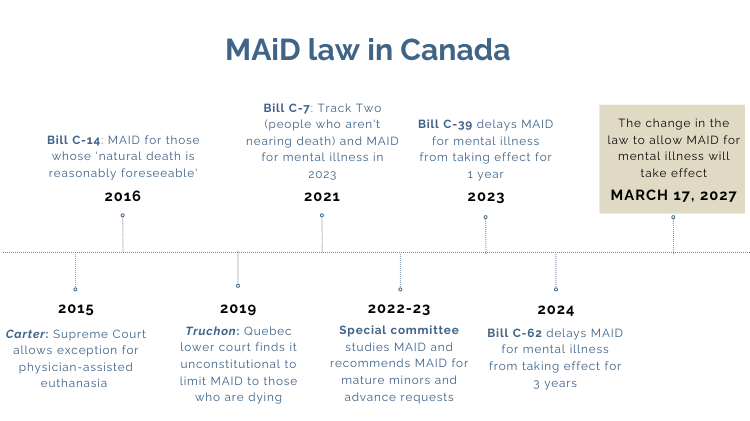 In 2015, the Supreme Court of Canada ruled physician-assisted dying could be allowed in certain circumstances. The EFC was an intervener in the Carter case, arguing for the sanctity of human life.
In 2015, the Supreme Court of Canada ruled physician-assisted dying could be allowed in certain circumstances. The EFC was an intervener in the Carter case, arguing for the sanctity of human life.
The federal government passed a law setting up medical assistance in dying (MAiD) in 2016. This initial law restricted MAiD to people nearing the end of life, whose natural death was “reasonably foreseeable” in the wording of the law. The law also required that a person be 18 years of age or older, capable of consent, and have a serious and incurable illness or disability. The EFC argued against Bill C-14, out of concern for vulnerable Canadians and that the law would move Canadian society away from a presumption for life.
In 2021, the government removed critical safeguards from the law. The most significant change was that Bill C-7 removed the previous requirement that a person’s death must be “reasonably foreseeable”, expanding MAiD to people with a disability or illness who are not dying. It also allowed euthanasia and assisted suicide for people on the basis of mental illness alone, with a delay built in before it would take effect. MAiD for mental illness has been delayed until March 2027. There are no additional safeguards in the legislation for people who are suffering solely from mental illness. The EFC opposed expanding the law and argued for the strictest possible safeguards to protect Canadians in vulnerable moments or situations.
A parliamentary committee that studied euthanasia and assisted suicide has also recommended removing the minimum age of eligibility, so that it is available to mature minors who are deemed capable of making a decision for MAiD. The committee also recommended allowing advance requests for euthanasia, which would mean that people could have their lives ended when they are no longer capable of consent. The EFC had strongly urged the committee not to expand euthanasia/assisted suicide further.
This is an important time to engage on MAiD for mental illness. Canadians will become eligible for MAiD on the basis of mental illness in March 2027 unless a bill is passed to stop it. Scroll further for more general EFC resources on MAiD. Feel free to reproduce and distribute these materials to your friends, family and church network.
Stop MAiD for mental illness
Ask your MP to support a new bill to stop MAiD for mental illness
Slides to share in your church
Ask for change
Write, call or meet with your MP to explain your concerns. To have a greater impact, contact your MP in more than one way – for example, write and call. Remember to be respectful and gracious.
Contact your local MP and ask them to take one or more of these actions:
- to stop MAiD for mental illness, for example by supporting Bill C-218
- to protect MAiD-free spaces
- to require conversations about MAiD be patient-initiated
- to oppose the expansion of MAiD to children and teens
- to oppose advance requests for MAiD
- to ensure palliative care is available to every Canadian who needs it
Find your MP’s contact information
here.
Pray
- For churches to reach out and demonstrate the love of Christ in tangible ways
- For those who are suffering and may feel life is not worth living
- For strength and wisdom for health care providers and institutions
- For elected officials to make decisions that affirms the value and dignity of human life wisdom and God-honouring decision-making from our elected officials
Learn and educate
Read and share the EFC’s updated brochures on the state of MAiD in Canada:
See the EFC’s booklet on palliative care:
Palliative Care Toolkit
Sign up for the
EFC Update weekly newsletter, EFC social media feeds, and/or the EFC bimonthly newsletter
Canada Watch